Infectious disease
Abstract
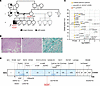
TB (Tuberculosis) and HIV co-infection remains a major global health challenge, with limited understanding of how these pathogens impact local immune responses in the lungs. This study is the first to investigate the modulation of IL-21 during LTBI and Mycobacterium tuberculosis (Mtb)/ Simian Immunodeficiency Virus (SIV) co-infection in non-human primates (NHP). We show that IL-21 expression, predominantly derived from CD4⁺ T cells, is significantly reduced in lungs of Mtb/SIV co-infected macaques, especially in the absence of cART. Although cART and cART with 3HP partially restore IL-21-producing CD4⁺ T cells, levels remain below those in LTBI, indicating ongoing immune impairment. Spatial transcriptomic analysis suggests localized alterations in immune signaling, including differences in STAT1- and STAT3-associated transcriptional profiles and reduced Mtb-specific IFN-γ responses in co-infected animals. Together, our findings indicate that IL-21-producing CD4⁺ T cells are selectively and persistently impaired in the lungs during Mtb/SIV co-infection despite antimicrobial and antiviral therapy. These results highlight a compartment-specific deficit in immune reconstitution and suggest that IL-21-associated pathways may warrant further investigation as potential targets for host-directed therapeutic strategies.
Authors
Vinay Shivanna, Renee D. Escalona, Colin Chuba, Shashi Prakash Singh, Ahmed A. Moustafa, J. Quincy Brown, Chenyao Xiao, Sangkyu Kim, Edward J. Dick Jr., Smriti Mehra, Mirko Paiardini, Riti Sharan
Abstract
BACKGROUND. Malaria caused by Plasmodium malariae is geographically widespread and sometimes associated with prolonged infection, yet little is known about its genomic epidemiology. METHODS. We performed hybrid capture and whole genome sequencing of 77 isolates collected from Cameroon (n=7), the Democratic Republic of the Congo (n=16), Nigeria (n=4), and Tanzania (n=50) between 2015 and 2021, and analyzing parasite genetic population structure and demography. RESULTS. There is no evidence of geographic population structure. Nucleotide diversity was significantly lower than in co-localized P. falciparum isolates, while linkage disequilibrium was significantly higher. Genome-wide selection scans identified no erythrocyte invasion ligands or antimalarial resistance orthologs as top hits; however, targeted analyses of these loci revealed evidence of selective sweeps around four erythrocyte invasion ligands and six antimalarial resistance orthologs. Demographic inference modeling suggests that African P. malariae is recovering from a bottleneck. CONCLUSION.P. malariae is genomically atypical among human Plasmodium spp. and lacks strong population structure in Africa. The low diversity has potential impacts on understanding persistent versus new infection through genomic epidemiology.
Authors
Zachary R. Popkin-Hall, Kelly Carey-Ewend, Farhang Aghakhanian, Eniyou C. Oriero, Misago D. Seth, Melchior M. Kashamuka, Billy Ngasala, Innocent M. Ali, Eric Mukomena SOMPWE, Celine I. Mandara, Oksana Kharabora, Rachel Sendor, Alfred Simkin, Alfred Amambua-Ngwa, Antoinette Tshefu, Abebe A. Fola, Deus S. Ishengoma, Jeffrey A. Bailey, Jonathan B. Parr, Jessica T. Lin, Jonathan J. Juliano
In Vivo Characterization of Candida Extracellular Vesicles Reveals Unique Infection Pathway Proteins
Abstract
Authors
Justin Massey, Robert Zarnowski, William Hartman Jr., Jeniel E. Nett, David R. Andes
Abstract
Inhibiting the mammalian target of rapamycin (mTOR) during acute viral infection generates highly functional memory CD8 T cells. We investigated the effects of inhibiting mTOR by using rapamycin during the effector and contraction phases of the immune response to a DNA prime and Modified Vaccinia Ankara (MVA) boost SIV vaccination in rhesus macaques. Rapamycin administered either during MVA boosts alone (DMR) or during both primes and boosts (DRMR) reduced the contraction of effector CD8 T cells, resulting in higher frequencies of SIV-specific memory CD8 T cells with enhanced quality as indicated by expression of Bcl-2 and CD127. Additionally, rapamycin reduced the frequency of proliferating CCR5+ CD4 T cells in the blood following the MVA boost. Post SIV251 infection, rapamycin-treated macaques demonstrated marked expansion of SIV-specific CD8 T cells (reaching up to 50% in blood and 25% in gut). The heightened expansion of SIV-specific CD8 T cells in the DMR group was associated with markedly lower (2-logs compared to unvaccinated and 1-log compared to DM) peak viral load in the gut and set-point viremia, along with improved survival post infection. Thus, inhibiting the mTOR pathway during MVA boosts of a DNA/MVA vaccine enhances vaccine efficacy by improving memory CD4 and CD8 T cell function.
Authors
Shanmugalakshmi Sadagopal, Kasey Stokdyk, Suefen Kwa, Rahul Basu, Sailaja Gangadhara, Rafi Ahmed, Smita S. Iyer, Koichi Araki, Rama Rao Amara
Abstract
Nearly 100 individuals have been identified who carry deleterious biallelic germline variants in CARD9 and experience life-threatening, invasive fungal infections caused by Ascomycetes but are otherwise resistant to other infectious agents. CARD9 is an adaptor protein expressed predominantly in myeloid cells, which functions downstream of dectin receptors, pattern recognition receptors for fungal antigens, to activate innate immune responses. The impact of CARD9 deficiency on lymphocytes, however, is less clear. We deciphered the functional consequences and delineated mechanisms of disease in a patient (P1) with a nonsense germline homozygous CARD9 variant (c.673A>T/p.K225*) and invasive Candida disease. P1’s PBMCs expressed truncated CARD9 and showed significantly reduced cytokine production in response to fungal ligands. P1 had reduced frequencies of circulating memory CD4+ TH17-like (CCR6+CXCR3–) cells. In addition, in vitro differentiation of P1’s naive CD4+ T cells into IL-17A/IL-17F–secreting cells was greatly impaired. Consistent with impaired responses of innate and adaptive immune cells from P1 in vitro, proportions of Candida-specific CD4+ T cells were strongly and selectively diminished. Our findings suggest that the CARD9 variant identified in P1 is pathogenic, affecting not only CARD9-induced immunity mediated by myeloid cells but also CD4+ T cell–intrinsic IL-17–dependent immunity and Candida-specific T cell responses.
Authors
Erika Della Mina, Carlos G. El-Haddad, Timothy A. West, Clara W.T. Chung, Jing Jing Li, Vivienne Lea, Elissa K. Deenick, Filomeen Haerynck, Jean-Laurent Casanova, Anne Puel, Cindy S. Ma, Stuart G. Tangye, Alisa Kane
Abstract
Natural killer (NK) cells are pivotal in the early immune response to Plasmodium falciparum infection, yet their functional dynamics and regulation remain incompletely understood. In a longitudinal study of malaria patients in a non-endemic setting, we observed a transient but potent activation of NK cell cytotoxicity during acute malaria, characterized by rapid granzyme B-mediated killing and elevated expression of genes associated with cytotoxicity (PRF1, GZMB, and GZMA). This heightened activity was supported by increased plasma levels of granzymes and proinflammatory cytokines, which enhanced NK cell function in vitro. However, plasma samples from clinical malaria also contained inhibitory mediators, including soluble cytokine receptors, which dampened NK cell responses. These findings reveal that the host microenvironment orchestrates a tightly regulated NK cell response that potentiates cytotoxicity during acute infection and rapidly downmodulate it after treatment. Understanding this balance between activation and suppression may inform strategies to harness NK cells for malaria control while minimizing immunopathology.
Authors
Pengjun Xi, Patrick A. Sandoz, Maximilian Julius Lautenbach, Eleni Bilev, Björn Önfelt, Anna Färnert, Quirin Hammer, Christopher Sundling
Abstract
BACKGROUND. Disseminated coccidioidomycosis (DCM) is an often fatal and otherwise intractable condition requiring lifelong antifungal treatment. We have previously shown that a deranged polarization of CD4+ T cells toward a Th2 phenotype can exist in the context of DCM. Here we studied a large population of subjects to determine the frequency of abnormal Th2 skewing of CD4+ T cells in patients with coccidioidomycosis and to identify underlying genetic mechanisms supporting this phenotype. METHODS. We collected peripheral blood mononuclear cells from 204 patients with coccidioidomycosis, including 96 patients with disseminated disease. We measured immune phenotypes and cytokine production by CD4+ T cells from patients and healthy controls, and comparisons between groups were made based on disease severity and demographics. Whole genome sequencing was conducted on 180 individuals who also had cytokine profiling. RESULTS. We found that ~25% of DCM patients had a CD4+ T-cell compartment that was abnormally skewed toward a Th2 phenotype, and Th2 skewing was highly correlated with male sex. Co-culture of T cells with the IL4R/IL13R-blocking antibody dupilumab reduced Th2 skewing. Sequencing revealed rare variants in genes involved in the IL-12-IFN-γ axis in several Th2-skewed patients, and we validated one such variant in IFNGR1 as hypomorphic. CONCLUSION. Patients with DCM, especially males, should be screened for Th2 skewing of CD4+ T cells. Patients with Th2 skewing should be additionally screened for genetic defects in the IL-12-IFN-γ axis. Our findings give a mechanistic rationale for blockade of IL4R in Th2-skewed patients with refractory coccidioidomycosis.
Authors
Timothy J. Thauland, Smriti S. Nagarajan, Alexis V. Stephens, Samantha L. Jensen, Anviksha Srivastava, Miguel A. Moreno Lastre, Terrie S. Ahn, Chantana Bun, Michael T. Trump, Royce H. Johnson, George R. Thompson III, Maria I. Garcia-Lloret, Valerie A. Arboleda, Manish J. Butte
Abstract
Background. Coccidioidomycosis ranges from self-limiting Uncomplicated Valley Fever (UVF) in most cases to life-threatening Disseminated Coccidioidomycosis (DCM) in rare individuals. A few patterns of immunologic deficits allowing for dissemination have been identified, though the specific defects in most individuals with DCM remain undefined. We hypothesized that chronic antigen exposure in DCM engenders a state of T cell exhaustion. Methods. From a cohort of over 300 subjects with confirmed diagnoses of coccidioidomycosis, circulating T cell phenotypes were characterized via flow cytometry and Coccidioides-specific T cell responses were measured by Activation-Induced Marker (AIM) assay. Results. Male sex was significantly associated with disseminated disease (odds ratio 2.5; 95% CI: 1.5 – 4.0). 52% of subjects showed Coccidioides-specific T cell responses in our AIM assay. We noted a significant difference in subjects sampled in the first year of diagnosis, where only 8% of DCM subjects had T cell responses during this time, as compared to 44% of UVF subjects (p = 0.04). Among DCM patients with detectable AIM responses, CD4+ T cells demonstrated an exhausted phenotype with elevated PD-1 expression compared to UVF subjects. In vitro PD-1 blockade augmented IFNγ production in most tested DCM subjects. Conclusion. These findings suggest that dissemination may occur in some individuals during a period of impaired antigen-specific T-cell activity. Importantly, these responses can be augmented in vitro by PD-1 blocking antibodies, supporting further study of immune checkpoint therapy as an adjunct to antifungal treatment in disseminated coccidioidomycosis.
Authors
Gregory D. Whitehill, Alexis V. Stephens, Timothy J. Thauland, Miguel A. Moreno Lastre, Matthew M. Tate, Sinem Beyhan, Royce H. Johnson, George R. Thompson III, Maria Garcia-Lloret, Manish J. Butte
Abstract
Antiretroviral therapy (ART) has prolonged the life expectancy of persons living with HIV, the majority of whom are now older than 50 years. Aging people with HIV are at increased risk for cardiovascular events driven by HIV-related inflammation and hypercoagulation. Apixaban is a factor Xa inhibitor that reduces cardiovascular risks and treats stroke, deep vein thrombosis, and pulmonary embolism. We assessed apixaban’s impact on key parameters of HIV/SIV pathogenesis in SIV-infected, aged rhesus macaques (RMs) receiving ART. Inflammation, coagulation, T cell subsets, B cells, and macrophages and their immune activation status were monitored throughout the study. We found no significant differences between the apixaban-treated and control groups for virus replication or CD4+ T cell recovery in blood and tissues after ART. Apixaban did not significantly affect D-dimer, immune activation, or inflammation of SIV-infected, ART-treated RMs. Apixaban-treated RMs experienced multiple bleeding episodes, tissue hemorrhages, and myocardial infarctions, as demonstrated by pathological examination of necropsy-collected tissues. Given apixaban’s lack of effect on immune activation, CD4+ T cell restoration, and inflammation, along with increased risk of hemorrhage, factor Xa inhibition may not be an efficient or safe option to target and prevent cardiovascular events in aging people with HIV.
Authors
Cuiling Xu, Haritha Annapureddy, Lilly Carson, Vansh Khurana, Ranjit Sivanandham, Sindhuja Sivanandham, Tianyu He, Kevin D. Raehtz, Janet Kim, Christie Biber, Norma Arbujas-Silva, Mohammed Daira, Sudhapriya Kandasamy, Matthew J. Feinstein, Irini Sereti, Cristian Apetrei, Ivona Pandrea
Abstract
Cytotoxic T lymphocytes form a critical component of SARS-CoV-2 immunity by recognizing viral peptides bound to HLA class I molecules. Here, we identified the Spike-derived peptide NYNYLYRLF448-456 (NF9) as the immunodominant HLA-A*24:02-restricted epitope in both convalescent and vaccinated donors. Across cohorts, A24/NF9-specific responses were dominated by public TCR motifs featuring TRAV12-1 (or TRAV6-1) paired with TRBJ2-7 and a conserved CDR3β sequence (CASSXXXGYEQYF). Using a panel of thirteen TCRs, we mapped recognition of single amino acid substitutions within NF9 and identified residue 5 (L452) as the principal determinant of escape. The L452R substitution, characteristic of the Delta variant, abolished recognition across all tested TCRs despite preserved HLA binding. Crystallography of a representative public TCR (P1-15) revealed that mutation at position 5 reoriented the peptide within HLA-A*24:02, flipping the adjacent Y453 side chain into the peptide-binding groove and eliminating the dominant TCR contact. This position-5-driven conformational switch provided a structural mechanism for universal loss of NF9 recognition by HLA-A*24:02-restricted T-cells. Consistent with this, Delta-infected convalescents failed to mount de novo NF9-5R-specific responses while retaining responses to the conserved A24/QI9 Spike epitope. Together, these findings defined the basis of A24/NF9 recognition and showed how one mutation remodelled peptide presentation to abrogate TCR responses.
Authors
Takeshi Nakama, Aaron Wall, Garry Dolton, Li-Rong Tan, Hannah Thomas, Hiroshi Hamana, Yoshiki Aritsu, Toong Seng Tan, Mako Toyoda, Yoshihiko Goto, Huanyu Li, Mizuki Kitamatsu, Keiko Udaka, Yusuke Miyashita, Hiroyuki Oshiumi, Kimitoshi Nakamura, Yoji Nagasaki, Rumi Minami, Hirotomo Nakata, Pierre J. Rizkallah, Hiroyuki Kishi, Takamasa Ueno, Andrew K. Sewell, Chihiro Motozono
No posts were found with this tag.