Autoimmunity
Abstract
BACKGROUND. Individuals with autoimmune diseases (AD) on immunosuppressants often have suboptimal responses to COVID-19 vaccine. We evaluated the efficacy and safety of additional COVID-19 vaccines in those treated with mycophenolate mofetil/mycophenolic acid (MMF/MPA), methotrexate (MTX), and B cell-depleting therapy (BCDT), including the impact of withholding MMF/MPA and MTX. METHODS. In this open-label, multicenter, randomized trial, 22 participants taking MMF/MPA, 26 taking MTX, and 93 treated with BCDT who had suboptimal antibody responses to initial COVID-19 vaccines (2 doses of BNT162b2 or mRNA-1273 or 1 dose of AD26.COV2.S) received an additional homologous vaccine. Participants taking MMF/MPA and MTX were randomized (1:1) to continue or withhold treatment around vaccination. The primary outcome was the change in anti-Wuhan-Hu-1 receptor-binding domain (RBD) concentrations at 4 weeks post-additional vaccination. Secondary outcomes included adverse events, COVID-19 , and AD activity through 48 weeks. RESULTS. Additional vaccination increased anti-RBD concentrations in participants taking MMF/MPA and MTX , irrespective of immunosuppressant withholding. BCDT-treated participants also demonstrated increased anti-RBD concentrations, albeit lower than MMF/MPA- and MTX-treated cohorts. COVID-19 occurred in 33% of participants; infections were predominantly mild and included only three non-fatal hospitalizations. Additional vaccination was well-tolerated, with low frequencies of severe disease flares and adverse events. CONCLUSION. Additional COVID-19 vaccination is effective and safe in individuals with ADs treated with immunosuppressants, regardless of whether MMF/MPA or MTX is withheld. TRIAL REGISTRATION. ClinicalTrials.gov (NCT05000216; registered August 6, 2021: https://clinicaltrials.gov/ct2/show/NCT05000216)
Authors
Meggan Mackay, Catriona A. Wagner, Ashley Pinckney, Jeffrey A. Cohen, Zachary S. Wallace, Arezou Khosroshahi, Jeffrey A. Sparks, Sandra Lord, Amit Saxena, Roberto Caricchio, Alfred H.J. Kim, Diane L. Kamen, Fotios Koumpouras, Anca D. Askanase, Kenneth Smith, Joel M. Guthridge, Gabriel Pardo, Yang Mao-Draayer, Susan Macwana, Sean McCarthy, Matthew A. Sherman, Sanaz Daneshfar Hamrah, Maria Veri, Sarah Walker, Kate York, Sara K. Tedeschi, Jennifer Wang, Gabrielle E. Dziubla, Mike Castro, Robin Carroll, Sandeep R. Narpala, Bob C. Lin, Leonid Serebryannyy, Adrian B. McDermott, William T. Barry, Ellen Goldmuntz, James McNamara, Aimee S. Payne, Amit Bar-Or, Dinesh Khanna, Judith A. James
Abstract
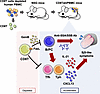
Peripheral helper T (Tph) and follicular helper T (Tfh) cells are key regulators of B cell differentiation and antibody production, making them promising targets for autoimmune disease treatment. However, their differentiation mechanisms differ significantly between humans and mice, limiting drug validation in mouse models. Here, we present a simple and effective method for in vivo proliferation of human Tph/Tfh and B cells. We discovered that after depleting CD8+ T cells of human peripheral blood mononuclear cell–transferred immunodeficient mice (CD8TΔhPBMC mice), human Tph/Tfh cells and B cells proliferated markedly in the spleen compared with those in human PBMC–transferred immunodeficient mice (hPBMC mice). Transcriptome analysis confirmed proliferating cells’ close resemblance to human Tph/Tfh cells. Furthermore, multicolor flow cytometry revealed CXCL13+ Tph cells infiltrating Sjögren’s syndrome–associated (SjS-associated) organs, such as salivary glands. Single-cell RNA sequencing identified IL-21+CXCL13+IFN-γ+ICOS+TIGIT+GPR56+ Tph cells in the salivary glands. These findings are consistent with reduced saliva volume and elevated SjS markers, such as anti-SSA antibody, in these mice, which were both ameliorated by immunosuppressants. In vitro, CD8+ T cells from hPBMC mice induced B cell apoptosis and inhibited Tph/Tfh differentiation. This model advances understanding of human Tph/Tfh cell biology and offers a valuable platform for studying SjS and therapeutic targets.
Authors
Mariam Piruzyan, Sota Fujimori, Ryota Sato, Yuki Imura, Sachiko Mochiduki, Kana Takemoto, Akiko Nishidate, Yuzo Koda
Abstract
Juvenile idiopathic arthritis (JIA) is the most prevalent chronic inflammatory arthritis of childhood, yet the spatial organization in the synovium remains poorly understood. Here, we perform subcellular-resolution spatial transcriptomic profiling of synovial tissue from patients with active JIA. We identify diverse immune and stromal cell populations and reconstruct spatially defined cellular niches. Applying a newly developed spatial colocalization analysis pipeline, we uncover microanatomical structures, including endothelial–fibroblast interactions mediated by NOTCH signalling, and a CXCL9-CXCR3 signaling axis between inflammatory macrophages and CD8+ T cells, alongside the characterization of other resident macrophage subsets. We also detect and characterize tertiary lymphoid structures marked by CXCL13-CXCR5 and CCL19-mediated signaling from Tph cells and immunoregulatory dendritic cells, analogous to those observed in other autoimmune diseases. Finally, comparative analysis with rheumatoid arthritis reveals JIA-enriched cell states, including NOTCH3+ and CXCL12+ sublining fibroblasts, suggesting potentially differential inflammatory programs in pediatric versus adult arthritis. These findings provide a spatially resolved molecular framework of JIA synovitis and introduce a generalizable computational pipeline for spatial colocalization analysis in tissue inflammation.
Authors
Jun Inamo, Roselyn Fierkens, Michael R. Clay, Anna Helena Jonsson, Clara Lin, Kari Hayes, Nathan D. Rogers, Heather Leach, Kentaro Yomogida
Abstract
Acute rheumatic fever (ARF) and associated rheumatic heart disease are serious sequelae of a Group A Streptococcus (GAS/Strep A) infection. Autoantibodies are thought to contribute to pathogenesis, with deeper exploration of the autoantibody repertoire needed to improve mechanistic understanding and identify new biomarkers. Phage immunoprecipitation and Sequencing (PhIP-Seq) with the HuScan library (>250,000 overlapping 90-mer peptides spanning the human proteome) was utilised to analyse autoreactivity in sera from children with ARF, uncomplicated Strep A pharyngitis and matched healthy controls. A global proteome-wide increase in autoantigen reactivity was observed in ARF, as was marked heterogeneity between patients. Public epitopes, common between individuals with ARF were rare, and comprised < 1% of all enriched peptides. Differential analysis identified both novel and previously identified ARF autoantigens, including PPP1R12B, a myosin phosphatase complex regulatory subunit expressed in cardiac muscle, and members of the collagen-protein family, respectively. Pathway analysis found antigens from the disease-relevant processes encompassing sarcomere and heart-morphogenesis were targeted. In sum, PhIP-Seq has substantially expanded the spectrum of autoantigens in ARF, and reveals the rarity of public epitopes in the disease. It provides further support for the role of epitope spreading in pathogenesis and has identified PPP1R12B as a novel, enriched autoantigen.
Authors
Reuben McGregor, Lauren H. Carlton, Timothy J. O'Donnell, Elliot Merritt, Campbell R. Sheen, Florina Chan Mow, William John Martin, Michael G. Baker, Nigel Wilson, Uri Laserson, Nicole J. Moreland
Abstract
The efficacy of anti-CD20 therapies places B cells and their interaction with T cells at the center of attention for multiple sclerosis (MS) pathogenesis. Follicular T helper cells (Tfh), which guide B cell maturation in germinal centers within lymph nodes (LNs), are elevated in the circulation and cerebrospinal fluid of patients with MS (pwMS). However, the LN spatial landscape has remained largely without investigation for pwMS. Using cyclic immunofluorescence, we assessed cell abundance and spatial connections in FFPE LNs of 33 pwMS and 35 non-MS controls. The presence of EBV was analyzed through EBER immunostaining and multiplex quantitative PCR. Our analysis showed that Tfh cells were expanded in LNs of pwMS and accumulated especially in the mantle zone and B cell follicles compared with controls. The Tfh/T follicular regulator ratio was increased in pwMS, while B cell ratios were similar between the cohorts. The interaction of Tfh cells with follicular B cells was higher in pwMS. Interestingly, Tfh accumulation was also observed in 5 prediagnostic MS cases. No signs of EBV latency were detected in either group. These findings highlight LNs as a site of early and persistent immune activation in pwMS, with therapeutic implications to be further addressed.
Authors
Joona Sarkkinen, Eliisa Kekäläinen, Leo Hannolainen, Ada Junquera, Johannes Dunkel, Maria F. Perdomo, Mikko I. Mäyränpää, Sini M. Laakso
Abstract
In the rheumatoid arthritis (RA) synovium, resident fibroblast-like synoviocytes (FLS) express MHC class II molecules (HLA-D) but lack the co-stimulatory signals typically required for T cell activation. Here, we demonstrate that antigen presentation by FLS induces a distinct T cell activation state characterized by high CD69, yet reduced CD25 and HLA-DR expression, suppressed proliferation, and decreased effector cytokine production compared to professional antigen presenting cells (APCs), such as macrophages. FLS were also capable of suppressing macrophage-induced T cell activation, underscoring their dominant immunomodulatory role in the synovial microenvironment. Mechanistically, we identify indoleamine 2,3-dioxygenase (IDO1)-mediated tryptophan depletion as the primary driver of FLS-induced T cell hypo-responsiveness. Spatial transcriptomics revealed colocalization of IDO1 and CD69 within ectopic lymphoid structures in RA synovium, further supporting the in vivo relevance of this pathway. These findings provide the groundwork for positioning FLS as critical T cell regulators in RA and highlight the importance of preserving their immunosuppressive properties when therapeutically targeting pathogenic FLS functions.
Authors
Melissa R. Romoff, Preethi K. Periyakoil, Edward F. DiCarlo, Daniel Ramirez, Susan M. Goodman, Christina S. Leslie, Alexander Y. Rudensky, Laura T. Donlin, Melanie H. Smith
Abstract
Rheumatoid arthritis (RA) is a common systemic autoimmune disorder. Fibroblast-like synoviocytes (FLS) have emerged as an attractive target for non-immunosuppressive RA therapy, but there are no approved drugs targeting FLS. The receptor protein tyrosine phosphatase sigma (PTPRS) negatively regulates FLS migration and has been proposed as a target for FLS-directed RA therapy. Here we examined the impact of sequence variations on efficacy of an FLS-targeted biologic comprised of Fc-fused PTPRS immunoglobulin (IgG)-like domains Ig1 and Ig2 (Ig1&2-Fc). Engineering the linker and Fc tag improved effectiveness of human Ig1&2-Fc in assays of FLS migration and a mouse model of arthritis. Treatment of mice with Ig1&2-Fc over four months revealed no signs of toxicity or organ pathology. Finally, we show potential of Ig1&2-Fc co-administration in combination or as a bispecific fusion with a tumor necrosis factor alpha inhibitor (TNFi). Combination treatment of mouse tumor necrosis factor receptor 2 (mTnfr2) with Ig1&2-Fc resulted in increased efficacy in suppressing arthritis beyond single agent treatment. When administered as a dual-action bispecific, Ig1&2 fused to mTnfr2 proved more efficacious at suppressing arthritis than mTnfr2 alone. This study illustrates the potential of Ig1&2-Fc as a combination or bispecific therapy with DMARDs to improve patient outcomes in RA.
Authors
Sterling H. Ramsey, Zixuan Zhao, Megan C. Lee, Thales Hein da Rosa, Ava C. Schneider, Miriam Bollmann, Nour Dada, Katie Frizzi, May M. Han, Jaeyeon Kim, Martina Zoccheddu, Nigel A. Calcutt, Gary S. Firestein, James W. Bryson, Mattias N.D. Svensson, Eugenio Santelli, Stephanie M. Stanford, Nunzio Bottini
Abstract
Mucous membrane pemphigoid (MMP) is a mucocutaneous autoimmune blistering disease affecting diverse mucous membranes and the skin with inflammatory blisters and erosions. The pathogenesis of MMP is only poorly understood, but inflammation in MMP is triggered by specific binding of autoantibodies directed to different proteins of the dermal-epidermal/-epithelial junction, subsequently leading to the influx of inflammatory cells, particularly neutrophils, into the dermis. Using the anti-laminin 332 antibody transfer model of MMP, we addressed the molecular mechanisms of neutrophil infiltration and its significance for the eruption of mucocutaneous lesions. Mice deficient in 5-lipoxygenase (Alox5–/–) or in the leukotriene B4 (LTB4) receptor BLT1 (Ltb4r1–/–) were resistant to skin inflammation and exhibited substantially fewer mucosal lesions, with deficiency in either gene compromising the recruitment of neutrophils to the lesion. Furthermore, neutrophil-specific genetic deficiency in Ltb4r1 similarly protected from MMP. Hence, BLT1 was required on neutrophils, and neutrophil recruitment was indispensable for the eruption of lesions in MMP. In line with these findings, the BLT1 inhibitor CP-105,606 ameliorated MMP dose-dependently. Collectively, our results highlight neutrophils and LTB4/BLT1 as key drivers of inflammation in MMP and as promising therapeutic targets.
Authors
Tabea Bremer, Sripriya Murthy, Sabrina Patzelt, Paul Schilf, Mareike Neumann, Sina Gonther, Jasper Pruessmann, Wiebke Pruessmann, Enno Schmidt, Thomas Rülicke, Christian D. Sadik
Abstract
Glutaminolysis is enhanced in T cells of lupus patients and in follicular helper T (Tfh) cells, a critical subset of CD4+ T cells that provide help to autoreactive B cells, in lupus mice. Glutaminolysis inhibitors reduced lupus activity in association with a decreased frequency of Th17 cells in mice. Here, we thought to determine the role of glutaminolysis in murine Tfh cells. The pharmacological inhibition of glutaminolysis with DON reduced the expression of the critical costimulatory molecule ICOS on lupus Tfh cells, in association with a reduction of autoantibody production and B cell differentiation markers. Accordingly, profound transcriptomic and metabolic changes, including a reduction of glycolysis, were induced by DON in lupus Tfh cells, whereas healthy Tfh cells showed minor changes. The T cell-specific genetic inhibition of glutaminolysis largely phenocopied the effects of DON on Tfh cells and B cells in an autoimmune genetic background with minor changes in Tfh and B cells in healthy controls. Furthermore, we showed that T cell-specific glutaminolysis inhibition impaired T-dependent humoral responses in autoimmune mice as well as their Tfh response to a viral infection. Overall, these results suggest that lupus Tfh cells have a greater intrinsic requirement of glutaminolysis for their helper functions.
Authors
Seung-Chul Choi, Yong Ge, Milind V. Joshi, Damian Jimenez, Abigail Castellanos Garcia, Cassandra LaPlante, Lauren T. Padilla, Chaoyu Ma, Nu Zhang, Jeffrey C. Rathmell, Mansour Mohamadzadeh, Laurence Morel
Abstract
In celiac disease (CeD), a gluten-dependent autoimmune disorder, transglutaminase 2 (TG2) deamidates selected glutamine residues in gluten peptides, while HLA-DQ2 presents deamidated antigens to inflammatory T cells. The cellular sources of pathogenic TG2 and DQ2 are unclear. Using chemical biology tools, we show that intestinal CD103+ dendritic cells (DCs) couple cell-surface TG2 to the endocytic LRP1 receptor to simultaneously deamidate gluten antigens and concentrate them in lysosomes. In DQ2-transgenic mice, CD103+ DCs loaded with deamidated antigens migrate from intestinal lamina propria and Peyer’s patches into mesenteric lymph nodes, where they engage T cells. In turn, gluten antigen presentation upregulates intestinal TG2 activity. The tool (HB-230) used to establish a role of CD103+ DCs in gluten antigen presentation and TG2 activation in mice also revealed that the TG2/LRP1 pathway is active in human CD14+ monocytes. Within this population of circulating monocytes, a DC subset with the gut-homing β7-integrin marker is elevated in CeD patients with active disease compared to non-celiac controls or patients on a gluten-free diet. Our findings not only inform the cellular basis for gluten toxicity in CeD but they also highlight the immunologic role of an enigmatic protein of growing therapeutic relevance in CeD and other immune disorders.
Authors
Fu-Chen Yang, Harrison A. Besser, Hye Rin Chun, Megan Albertelli, Nielsen Q. Fernandez-Becker, Bana Jabri, Chaitan Khosla
No posts were found with this tag.